Becoming the Sage: What Perimenopause Is Really Asking of You
By Dr. Michele Renee, DC, MAc, LMT
READ TIME 10 MINUTESButterfly with many coccoons. Transformation, healthy aging, vitality, honoring the body, self-care, aging gracefully, integrative care, holistic healthcare, tendonitis, hot flashes, night sweats
If you've found yourself lying awake at 3am drenched in sweat, snapping at people you love for reasons you can't quite explain, or crying in the car on the way to work and genuinely wondering what is happening to you — this is for you.
You are not falling apart. You are in perimenopause. And your body is doing something enormous.
What Is Actually Happening
Perimenopause is the transition phase leading up to menopause — the point when menstrual cycles have stopped for 12 consecutive months. This transition can begin anywhere from your late 30s to your mid-50s, and it typically lasts somewhere between four and ten years. For many people, it starts much earlier than they expected.
The hormonal shifts driving this transition are real, measurable, and significant. Estrogen and progesterone — which have been orchestrating a monthly rhythm in your body for decades — begin to fluctuate in less predictable patterns. Estrogen in particular doesn't simply decline in a steady, graceful arc. It surges. It drops. It fluctuates wildly before it eventually settles lower. Progesterone tends to fall more consistently and earlier. That estrogen-to-progesterone imbalance, often called "estrogen dominance," accounts for many of the most disruptive symptoms in early perimenopause.
Meanwhile, the hypothalamic-pituitary-ovarian axis — the feedback loop between your brain and your ovaries — is recalibrating. That recalibration touches almost every system in your body: cardiovascular, neurological, musculoskeletal, gastrointestinal, immune. Perimenopause is not a reproductive event with a few side effects. It is a whole-body transition.
How It Feels
There's a reason so many people describe perimenopause as confusing before they describe it as difficult. The symptoms are wildly varied, often unpredictable, and frequently dismissed — including by well-meaning healthcare providers.
Here's what the research, and what our patients, tell us this transition can look like:
The classics:
Hot flashes and night sweats (collectively called vasomotor symptoms) are the most recognizable. They're caused by the hypothalamus becoming more sensitive to small changes in body temperature as estrogen levels shift. For some people these are mild and occasional. For others, they are relentless and sleep-destroying.
The ones that catch you off guard:
Sleep disruption, even on nights without obvious night sweats.
Brain fog — that unsettling sense that words are slower to come, focus harder to sustain, memory less reliable.
Mood changes: anxiety that seems to come from nowhere, irritability that feels disproportionate, a low mood that can shade into depression
Joint aches
Heart palpitations
Changes in digestion
The emotional ones that feel like they're coming from nowhere:
Anger that flares hot and fast
Weepiness that arrives without an obvious trigger
A moodiness that makes you feel like a stranger in your own life — or like you're somehow failing at being the person everyone around you needs you to be.
These symptoms are real, they are physiological, and they are profoundly under-acknowledged.
Here's a frame that might help: perimenopause is, in many ways, adolescence in reverse. The same hormonal architecture — fluctuating estrogen, dropping progesterone, a nervous system recalibrating in real time — that drove the emotional intensity of your teenage years is happening again, but moving in the other direction. If you were moody and tearful and sometimes explosive at 14, and nobody questioned whether something was wrong with you, the same grace applies now.
But unlike adolescence, perimenopause often happens in the middle of a life full of responsibilities — a career, relationships, children or aging parents or both, a community counting on you. There isn't much cultural permission to be in a tender, turbulent transition when everyone needs you to be stable. That gap — between what your body is doing and what your life demands — is where the loneliness lives.
What we don't talk about enough is that this transition also carries an invitation.
Wise woman with head covering, lined face, integrative care, whole person care, honoring life stages, maiden - mother - sage.
Many traditions have named this passage: the movement from the Mother archetype — the years of fertility, caregiving, outward orientation, and generativity, whether or not you chose biological motherhood — toward the Sage, or what older traditions called the Crone. Not diminishing. Not decline. A different kind of power: accumulated wisdom, less tolerance for what doesn't matter, a clarifying relationship with your own values and voice.
We honor menarche (or we should) as a threshold crossing — a girl becoming a young woman, her body announcing a new chapter. Menopause deserves the same reverence. You are not losing something. You are crossing into something. The anger and grief and intensity that can accompany this time may be part of the threshold, not evidence that you're broken.
Strong powerful Black woman smiling. Transition, respect, aging gracefully, sage, integrative care.
This doesn't make the hot flashes less real or the 3am anxiety less exhausting. But meaning matters. Having a frame for what's happening — biologically, emotionally, and archetypally — can make it less isolating, and more navigable.
The ones nobody warned you about: Skin and hair changes. Shifts in libido. Vaginal dryness that affects comfort and intimacy. Urinary frequency or urgency. Changes in how you respond to stress — things that used to roll off you now feel unbearable.
None of this is in your head. All of it has physiological roots. And all of it is worth taking seriously.
The Joints and Tendons Nobody Warned You About
Here's something that doesn't make the standard list of perimenopause symptoms, even though it probably should: your body hurts in new ways. Your hip aches after a walk. Your shoulder freezes up seemingly overnight. Your heel is suddenly sore every morning. You've been active for decades — nothing has changed about how you move — and now everything feels different.
This is not a coincidence.
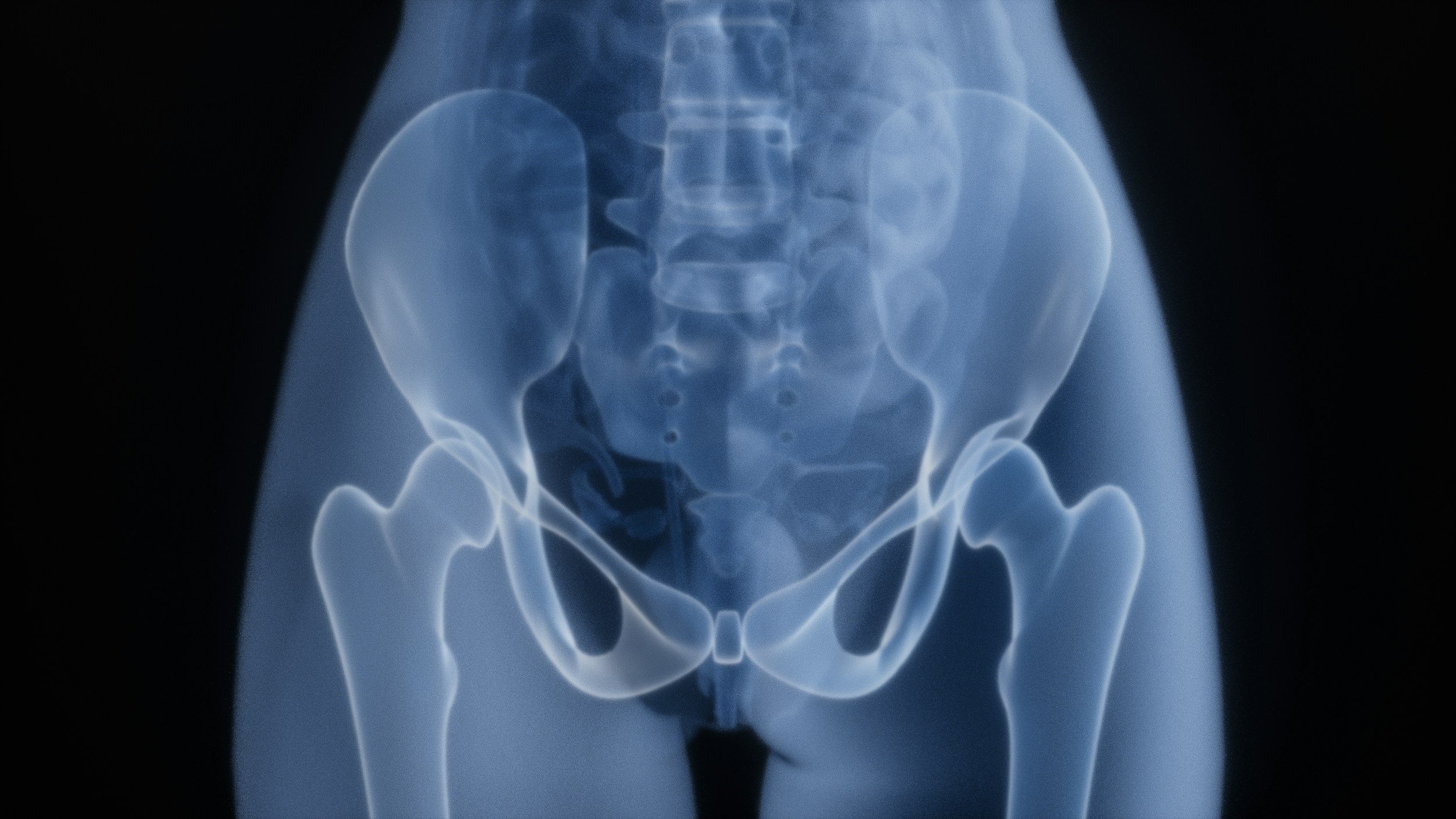
Imaging of pelvis, hip pain, gluteal tendinopathy, collagen synthesis, muscle loss, connective tissue change, integrative care for perimenopause, holistic healthcare
In October 2024, researchers formally introduced the term "musculoskeletal syndrome of menopause" to describe exactly this cluster of symptoms — joint pain, tendon irritability, muscle loss, and connective tissue changes driven by hormonal shifts. Studies estimate that up to 70% of people going through perimenopause experience these symptoms, and nearly a quarter find them debilitating. Most of them have no idea their hormones are involved.
Why Estrogen Matters for Connective Tissue
Estrogen does far more than regulate reproductive cycles. Estrogen receptors are found throughout the musculoskeletal system — in joints, ligaments, tendons, and bones. Estrogen is also a powerful anti-inflammatory agent, actively suppressing pro-inflammatory signaling molecules including IL-6 and TNF-alpha. When estrogen levels begin to fluctuate and decline, that anti-inflammatory protection drops — and the whole connective tissue system feels it.
Here's what's happening at the tissue level: tendons are primarily made of collagen, and estrogen plays a direct role in collagen synthesis and maintenance. As estrogen fluctuates, collagen production slows, tendons lose elasticity, and the body's ability to repair the small micro-tears of daily activity becomes impaired. Tendons that were quietly managing everyday load become irritable, stiff, and slow to heal. Meanwhile, the systemic increase in inflammatory cytokines lowers the pain threshold — so conditions that might have been asymptomatic before suddenly hurt.
The Specific Conditions We See
Gluteal tendinopathy is one of the most common and underrecognized presentations. It's frequently misdiagnosed as hip bursitis — a sharp or aching pain on the outer hip, sometimes radiating down the thigh, that worsens with sitting, crossing the legs, or climbing stairs. This is a tendinopathy of the gluteal medius and minimus, and it has a well-documented relationship with perimenopause. The combination of estrogen-mediated collagen changes, reduced muscle mass (also driven by hormonal shifts), and increased inflammatory load creates the perfect conditions for these tendons to break down.
Frozen shoulder (adhesive capsulitis) disproportionately affects women between 40 and 60, and emerging research points to estrogen withdrawal as an important contributing factor.
Plantar fasciitis, Achilles tendinopathy, and rotator cuff irritation follow similar patterns — showing up in people who have been active for years without these issues, at precisely the time their hormones are shifting.
The characteristic feature of the musculoskeletal syndrome of menopause that distinguishes it from straightforward overuse injuries or osteoarthritis: the pain tends to move around. Different joints at different times. Widespread aching that doesn't fit a clean structural diagnosis. If that sounds familiar, the hormonal connection is worth taking seriously.
What This Means for Care
The integrative approach matters enormously here. You can't separate the tendon from the hormonal environment it lives in. Treating gluteal tendinopathy without acknowledging estrogen's role, or addressing joint pain without considering inflammation as a system-wide phenomenon, is incomplete care.
Progressive loading and strength training are essential — tendons respond to load, and building the surrounding musculature reduces the demand on compromised connective tissue.
Anti-inflammatory nutrition support makes a meaningful difference in the tissue environment.
Acupuncture has evidence for both pain modulation and systemic inflammatory regulation.
And for some people, addressing the hormonal root through bioidentical or conventional hormone therapy is what finally allows the tendons to heal.
Most importantly: if you've developed tendon or joint pain in your 40s or 50s and you're also noticing other perimenopausal symptoms, please tell your provider. The timing is not a coincidence. You deserve care that sees the whole picture.
Woman with white hair sitting in lotus position with hands in prayer position. Integrative care, holistic medicine, whole person healthcare, person centered. Individualized care for life transitions, perimenopause, menopause, hot flash, disturbed sleep, botanicals, manual therapy, Chinese medicine
An Integrative Perspective
At Stockheart, we don't think about perimenopause as a deficiency to be corrected. We think about it as a transition that requires conditions — specific, tended conditions — for the body to move through with as much ease as possible.
That means we look at the whole picture.
Nervous System First
Many of the most uncomfortable perimenopausal symptoms are amplified by a nervous system running in chronic stress activation. When cortisol is high and the adrenals are already working overtime, the hormonal fluctuations of perimenopause hit harder. The hot flash that might have been mild becomes intense. The anxiety that might have been manageable becomes overwhelming.
Nervous system support is foundational. This is where acupuncture does some of its most meaningful work in perimenopause — regulating the hypothalamic-pituitary axis, modulating vasomotor symptoms, and shifting the body toward parasympathetic tone. Multiple systematic reviews support acupuncture's effectiveness for hot flashes, sleep disruption, and mood stabilization during this transition. We see it in our clinic consistently.
Chiropractic care addresses the structural and neurological load the body is carrying — because perimenopause often coincides with years of accumulated tension, previous injuries, and postural patterns that are now showing up as neck pain, jaw tightness, or back pain that flares with each hormonal shift.
Massage therapy isn't a luxury during this time. It's a direct intervention for nervous system regulation, cortisol reduction, and the kind of embodied settling that many perimenopausal people desperately need.
Blood Sugar and Inflammation
Estrogen has significant anti-inflammatory and blood-sugar-regulating effects. As it fluctuates and eventually declines, blood sugar instability and systemic inflammation can both increase. This shows up as fatigue, brain fog, mood swings, worsened hot flashes, and joint pain.
From a nutrition standpoint, this is the time to stabilize blood sugar with every meal — adequate protein, healthy fats, fiber, and a reduced load of refined carbohydrates and sugar. Magnesium, omega-3 fatty acids, and phytoestrogen-rich foods (flaxseed, soy, legumes) have meaningful evidence behind them for perimenopausal symptom support. An integrative nutritionist can help you build a food-as-medicine approach tailored to your specific presentation.
Sleep is Non-Negotiable
Sleep deprivation makes everything worse — hormones, mood, inflammation, cognitive function, pain. And perimenopause disrupts sleep through multiple pathways simultaneously: night sweats, increased cortisol, changes in progesterone (which has sleep-promoting properties), and shifts in circadian rhythm regulation.
Supporting sleep means addressing all the layers: the physical (temperature regulation, nervous system tone), the hormonal (sometimes botanical or bioidentical support), and the behavioral (sleep hygiene that actually works for a perimenopausal body).
The Conversation About Hormones
We believe in informed, individualized decision-making. Hormone therapy — including bioidentical hormone replacement — is a legitimate and often deeply helpful option for many people, and the decades-old fears about it have been significantly revised by more recent research. It's not right for everyone, and it's not the only option. But for people with significant vasomotor symptoms, sleep disruption, genitourinary changes, or mood destabilization, hormone therapy can be genuinely life-changing.
This is a conversation worth having with a provider who takes your symptoms seriously and understands the nuance. We're happy to be part of that conversation, and to collaborate with your primary care provider or OB/GYN.
Herbs, botanical support, holistic healthcare, integrative care, natural healing, perimenopause, menopause support, chiropractic, acupuncture, massage, nutrition, functional medicine
Botanical and Supplement Support
There is a meaningful body of evidence for several botanicals in perimenopause symptom management. Black cohosh has the strongest research base for vasomotor symptoms. Ashwagandha supports HPA axis regulation and stress resilience. Vitex (chaste tree berry) can help with progesterone-related symptoms in earlier perimenopause. Red clover and soy isoflavones provide phytoestrogenic support. Magnesium glycinate supports sleep, mood, and muscle tension.
These are not substitutes for addressing root causes, and they aren't one-size-fits-all. But used thoughtfully and in the right combinations, they can make a significant difference in quality of life.
What We Want You to Hear
You don't have to white-knuckle your way through this.
You don't have to accept that this is just what getting older feels like, or that your only options are to suffer or to medicate.
Your body is not betraying you. It is changing — significantly, systemically, in ways that deserve real attention and real care.
At Stockheart, we bring functional medicine, chiropractic, acupuncture, massage, and nutrition together because perimenopause asks for exactly that kind of whole-person approach. We meet you where you are. We collaborate with other providers. We take your symptoms seriously. And we help you build the conditions your body needs to move through this transition with more ease.
If any of this sounds familiar, we'd love to talk. Request a consultation and let's figure out what support would actually help.
Stockheart Whole Health is an integrative clinic in Minneapolis offering chiropractic, acupuncture, massage therapy, and nutritional support. We specialize in whole-person care for people navigating complex, whole-body transitions.
Michele Renee DC, MAc
A note from Dr. Michele:
I wrote this piece because I'm living it. I'm in perimenopause right now — navigating the night sweats, the mood shifts, the moments of wondering who I'm becoming. And I'm doing what I'd recommend to any of my patients: I'm using all of it. Maybe this is TMI, but I think it helps to share our stories, so here it is. I’m utilizing HRT, herbs, acupuncture, massage, chiropractic care. Not because I have it all figured out, but because my body deserves the same tending I've spent my career helping others find.
Writing this felt important, especially as Mother's Day approaches. Whatever motherhood has meant in your life — chosen or not, biological or not, celebrated or complicated — you have been in a season of pouring outward. This transition is asking something different of you. I'm in it with you.
— Dr. Michele Renee, DC, MAc, LMT